Facing the prospect of gallbladder surgery can feel overwhelming. Many patients experience abdominal pain, digestive discomfort, or repeated gallstone attacks before surgery. Questions often arise: How is the procedure performed? How long will recovery take? What changes should I expect in digestion afterward?
Gallbladder removal surgery, medically known as cholecystectomy, is one of the most commonly performed procedures in the United States. While the surgery is generally safe and effective, understanding every stage—from preoperative preparation to long-term recovery—can help patients feel more confident and reduce anxiety.
This comprehensive guide explains gallbladder removal surgery, including when it is recommended, the different surgical approaches, what to expect during recovery, potential complications, and lifestyle adjustments that support digestive health.
What Is the Gallbladder and Why Surgery Is Sometimes Needed
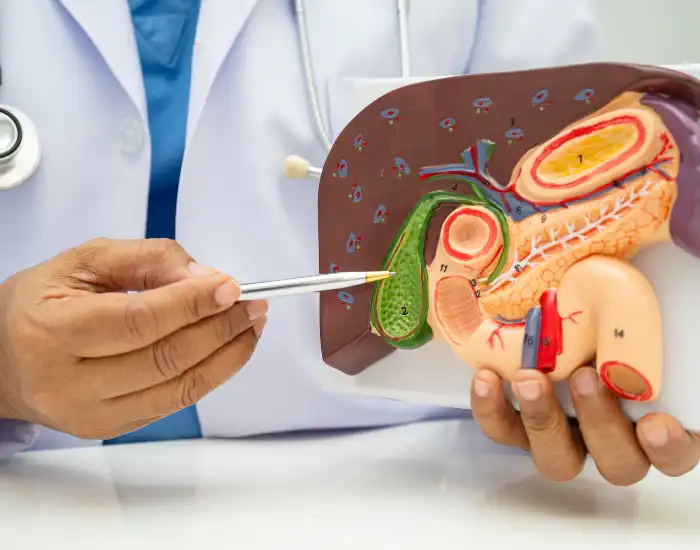
The gallbladder is a small, pear-shaped organ located under the liver in the upper right abdomen. Its main function is to store and concentrate bile, a digestive fluid produced by the liver that helps break down fats.
While the gallbladder is helpful, it is not essential. The liver continues to produce bile even if the gallbladder is removed. However, certain conditions can make gallbladder removal necessary:
Common Reasons for Gallbladder Removal
- Gallstones: Hardened deposits in the gallbladder that can block bile flow, causing pain or digestive issues.
- Cholecystitis: Inflammation of the gallbladder, often triggered by gallstones, infection, or bile buildup.
- Gallbladder polyps or tumors: Abnormal growths that may increase the risk of cancer.
- Biliary dyskinesia: Poor gallbladder function causing digestive discomfort.
- Pancreatitis: Inflammation of the pancreas caused by gallstones blocking bile ducts.
Patients often wonder if surgery is their only option. While some minor gallbladder issues can be managed conservatively with dietary adjustments or medication, recurrent attacks, severe pain, or complications usually necessitate surgical removal.
Types of Gallbladder Removal Surgery
There are two main approaches to gallbladder removal surgery. Each method has its benefits and may influence recovery time.
Laparoscopic Cholecystectomy
Laparoscopic surgery is the most common method. It involves:
- Several small incisions in the abdomen
- Insertion of a tiny camera and surgical instruments
- Removal of the gallbladder through one of the small incisions
Benefits of laparoscopic surgery include:
- Shorter hospital stay (often outpatient or 24 hours)
- Less postoperative pain
- Faster recovery and return to normal activities
- Smaller scars
Most patients are able to resume light activity within a few days and return to work within one to two weeks.
Open Cholecystectomy
Open surgery is performed through a larger incision in the abdomen. It is usually reserved for:
- Patients with severe inflammation or infection
- Complicated gallstones or anatomical challenges
- Previous abdominal surgeries that make laparoscopic access difficult
Recovery from open surgery is longer, typically 4–6 weeks for full activity. While open surgery may involve more discomfort initially, it remains a safe and effective procedure when required.
Preparing for Gallbladder Removal Surgery
Preparation can help reduce anxiety and improve outcomes. Your surgeon will provide specific instructions, but common preoperative steps include:
- Medical evaluation: Blood tests, imaging studies (ultrasound or CT), and review of medications.
- Fasting: Avoiding food or drink for a certain period before surgery.
- Medication adjustments: Some medications may need to be paused, such as blood thinners.
- Lifestyle adjustments: Maintaining hydration, managing chronic conditions, and stopping smoking if applicable.
Understanding the procedure and asking questions about anesthesia, incision sites, and expected recovery can help patients feel more confident before surgery.
What to Expect During Surgery
Gallbladder removal surgery is typically performed under general anesthesia, meaning patients are asleep and pain-free during the procedure.
Laparoscopic Surgery Steps
- Small incisions are made in the abdomen.
- A laparoscope (tiny camera) is inserted for visualization.
- Surgical instruments remove the gallbladder.
- Bile ducts and surrounding tissues are checked for complications.
- Incisions are closed with sutures or surgical glue.
The procedure usually lasts
30–90 minutes, depending on complexity.
Open Surgery Steps
- A larger incision is made in the upper right abdomen.
- The gallbladder is carefully separated from surrounding tissues and removed.
- Incision is closed with sutures or staples.
Hospital stays are longer for open surgery, typically 2–3 days, but both approaches are highly effective in resolving gallbladder-related problems.
Recovery After Gallbladder Removal Surgery
Recovery experiences vary depending on the surgical method, overall health, and adherence to postoperative guidelines.
Immediate Recovery
- Patients are monitored in the hospital or outpatient setting for a few hours to ensure stable vital signs.
- Pain is managed with prescribed medications.
- Early walking is encouraged to reduce the risk of blood clots and promote circulation.
First Week
- Mild abdominal soreness and fatigue are common.
- Small, frequent meals are recommended to reduce digestive discomfort.
- Incisions should be kept clean and dry.
Weeks Two to Four
- Light activity and walking can resume gradually.
- Most patients return to work within 1–2 weeks after laparoscopic surgery; open surgery may require longer.
- Patients should continue avoiding heavy lifting or strenuous activity.
Full Recovery
- Most patients regain full activity within 4–6 weeks after open surgery and 2–4 weeks after laparoscopic surgery.
- Some digestive adjustments may persist temporarily, such as mild diarrhea or bloating after fatty meals.
Potential Short-Term and Long-Term Effects
Understanding potential effects helps patients recognize normal healing versus complications.
Short-Term Effects
- Pain or soreness near incision sites
- Bruising or swelling
- Temporary changes in bowel habits
- Mild nausea
Long-Term Effects
While many patients recover without significant issues, some may experience:
- Digestive changes: Difficulty tolerating fatty foods, occasional diarrhea, bloating
- Postcholecystectomy syndrome: Persistent abdominal discomfort, nausea, or bloating months or years after surgery
- Bile duct complications: Rare issues such as retained stones or bile duct narrowing
Most long-term effects are manageable with dietary adjustments, medication, or minimally invasive procedures if needed.
Diet and Lifestyle After Gallbladder Removal
Dietary changes can help the body adjust and minimize discomfort.
- Eat smaller, more frequent meals instead of large meals.
- Limit high-fat foods to reduce bloating and diarrhea.
- Gradually reintroduce fiber to support digestion.
- Stay hydrated to aid bowel function.
- Maintain regular physical activity to support overall health.
Most patients find that their digestive system adapts over time, and they can enjoy a normal diet without significant restrictions.
Signs That Require Medical Attention
Patients should contact a healthcare provider if they experience:
- Persistent or worsening abdominal pain
- Fever or chills
- Yellowing of the skin or eyes (jaundice)
- Persistent nausea or vomiting
- Severe diarrhea or dehydration
- New lumps or swelling at incision sites
Early evaluation ensures that potential complications such as infections or bile duct issues are promptly addressed.
Who Should Manage Gallbladder Health and Recovery
Several healthcare professionals may be involved:
Primary Care Physician
- Initial evaluation of symptoms
- Orders tests and refers to specialists
Gastroenterologist
- Manages ongoing digestive symptoms
- Evaluates bile flow and potential postcholecystectomy syndrome
General Surgeon
- Performs gallbladder removal surgery
- Evaluates and treats surgical complications
- Provides guidance on long-term digestive health
For patients searching online, looking for a
general surgeon near me can connect them with experienced professionals who perform minimally invasive gallbladder surgeries.
FAQs About Gallbladder Removal Surgery
- Is gallbladder surgery safe? Yes, it is generally safe with a high success rate.
- Will I have digestive problems after surgery? Some mild adjustments are normal; most patients adapt over time.
- How long will I be in the hospital? Laparoscopic surgery is often outpatient; open surgery usually requires 2–3 days.
- When can I return to work? Light work may resume in 1–2 weeks; heavy labor may take 4–6 weeks.
Preparing for a Smooth Recovery
- Follow pre- and postoperative instructions carefully.
- Arrange for help at home if needed in the first few days.
- Avoid smoking and maintain a healthy lifestyle to promote healing.
- Schedule follow-up appointments to monitor recovery.
These steps support faster healing and minimize complications.
Conclusion
Gallbladder removal surgery is a highly effective treatment for gallstones, inflammation, and other gallbladder-related conditions. Most patients recover smoothly and return to normal activities within a few weeks. Understanding the procedure, recovery expectations, dietary adjustments, and potential long-term effects helps patients feel prepared and confident throughout the process.
Persistent symptoms, postcholecystectomy syndrome, or bile duct complications may require follow-up care. Consulting a primary care physician, gastroenterologist, or
general surgeon near me ensures timely evaluation and proper management.
With proper care, patients can maintain digestive health and enjoy life without the gallbladder.
Medical Disclaimer: This article is for educational purposes only and does not replace professional medical advice, diagnosis, or treatment. Individuals considering or recovering from gallbladder removal surgery should consult a qualified healthcare professional for personalized evaluation and guidance.