Gallbladder surgery is one of the most commonly performed procedures in the United States. Many patients expect immediate relief from gallstones, abdominal pain, or digestive issues. For most, surgery is highly effective. However, some individuals may experience digestive changes or other issues long after gallbladder removal.
It is natural to wonder: what are the long-term effects of gallbladder removal, and how will this procedure impact daily life over the years? Understanding the possible outcomes can help patients recognize normal adjustments, identify potential complications, and make informed decisions about diet, lifestyle, and follow-up care.
This guide explains what patients may experience years after gallbladder surgery, why these changes happen, and when medical evaluation may be necessary.
What Happens After Gallbladder Removal
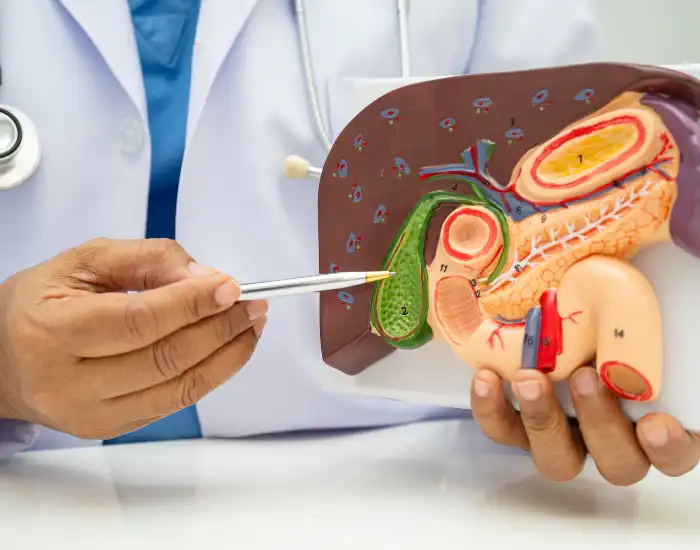
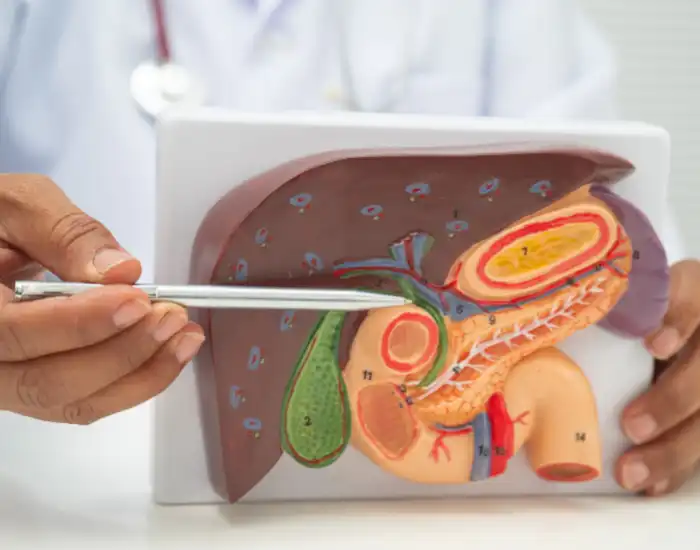
The gallbladder is a small organ beneath the liver that stores bile, a digestive fluid that breaks down fats. After gallbladder removal, bile flows directly from the liver into the small intestine instead of being stored.
For most patients, this change is well-tolerated. The liver continues producing bile, and digestion remains effective. However, some long-term adjustments may occur, leading to symptoms that prompt questions about the long-term effects of gallbladder removal.
Common Long-Term Digestive Effects
Many patients notice mild digestive changes that persist for months or years. Common long-term effects include:
- Changes in bowel habits: Some patients experience diarrhea or loose stools, particularly after fatty meals.
- Fat intolerance: Certain foods high in fat may cause bloating, gas, or discomfort.
- Bloating and gas: Altered bile flow can sometimes contribute to increased gas or abdominal fullness.
- Acid reflux or heartburn: Some individuals develop occasional reflux symptoms post-surgery.
These digestive adjustments are usually manageable with dietary modifications and lifestyle strategies.
Postcholecystectomy Syndrome
A subset of patients develops a condition known as postcholecystectomy syndrome, where digestive symptoms continue or appear years after surgery. Symptoms may include:
- Persistent abdominal pain
- Nausea or vomiting
- Chronic diarrhea
- Indigestion or bloating
- Fat intolerance
Causes of postcholecystectomy syndrome may include:
- Retained or migrated bile duct stones
- Narrowing or scarring of bile ducts
- Sphincter of Oddi dysfunction affecting bile flow
- Other digestive disorders unrelated to surgery
Diagnosis typically involves blood tests, imaging, and sometimes endoscopic evaluation. Treatment varies depending on the underlying cause and may include medication, dietary adjustments, or minimally invasive procedures.
Nutritional Considerations After Gallbladder Removal
Understanding the long-term effects of gallbladder removal includes recognizing how digestion may change:
- Small, frequent meals: Eating smaller meals throughout the day can reduce digestive discomfort.
- Moderate fat intake: Limiting high-fat foods helps prevent bloating, diarrhea, or cramping.
- Balanced diet: Incorporating fiber, lean protein, and vegetables supports healthy digestion.
- Hydration: Drinking enough water aids digestion and prevents constipation.
These strategies help the body adapt to the absence of the gallbladder and minimize long-term digestive effects.
Rare but Serious Long-Term Complications
Although uncommon, some patients may develop complications that require medical attention years after surgery:
- Bile duct obstruction or strictures: Scar tissue or retained stones can block bile flow.
- Chronic diarrhea or bile acid malabsorption: Ongoing irritation from bile acids may require medical management.
- Gallbladder-related cancer is no longer a concern, but other digestive conditions may mimic gallbladder symptoms.
Patients experiencing persistent pain, jaundice, unexplained weight loss, or other concerning symptoms should seek evaluation from a qualified physician or search for a general surgeon near me.
Who Can Help Manage Long-Term Effects
Several healthcare professionals may play a role in evaluating and managing the long-term effects of gallbladder removal:
Primary Care Physician
- Performs initial evaluation of ongoing digestive symptoms
- Orders basic blood tests and imaging
- Refers patients to specialists if needed
Gastroenterologist
- Evaluates chronic digestive symptoms
- Manages conditions like bile acid diarrhea, reflux, or postcholecystectomy syndrome
General Surgeon
- Evaluates structural complications related to surgery
- Provides interventions if bile ducts or other surgical issues are involved
Seeking care from the right specialist can provide clarity and help patients manage long-term symptoms effectively.
Lifestyle Tips to Minimize Long-Term Effects
Even years after gallbladder removal, certain habits can support digestive health:
- Maintain a healthy weight to reduce abdominal pressure
- Exercise regularly to promote digestion and overall wellness
- Eat a balanced diet with moderate fat
- Avoid excessive alcohol or irritants that may worsen digestion
- Monitor symptoms and seek medical advice promptly when new issues arise
These lifestyle choices can help reduce the long-term effects of gallbladder removal and improve overall quality of life.
When to Seek Medical Evaluation
Long-term digestive changes are often mild, but medical attention is important when symptoms include:
- Persistent or worsening abdominal pain
- Yellowing of the skin or eyes (jaundice)
- Chronic diarrhea affecting daily life
- Sudden unexplained weight loss
- Fever or signs of infection
Timely evaluation allows doctors to rule out complications and provide effective treatment options.
Conclusion
Gallbladder removal is generally safe and effective. Most patients recover fully and experience few long-term issues. However, understanding the long-term effects of gallbladder removal helps patients recognize normal digestive adjustments, identify potential complications, and make informed lifestyle choices.
Persistent digestive symptoms, postcholecystectomy syndrome, or bile duct issues may require medical evaluation. Consulting a primary care physician, gastroenterologist, or general surgeon ensures that long-term digestive health is maintained. With proper care, most individuals enjoy normal digestion and a high quality of life years after gallbladder removal.
Medical Disclaimer: This content is for educational purposes only and does not replace professional medical advice, diagnosis, or treatment. Individuals experiencing symptoms or concerns related to the long-term effects of gallbladder removal should consult a qualified healthcare professional for personalized evaluation and guidance.